 Medisage Medical
Medisage Medical
 Medisage Medical
Medisage Medical
Understanding what is the difference between internal and external fixation is crucial for medical professionals and patients alike. Both techniques serve to stabilize bone fractures and facilitate proper healing. Internal fixation involves the use of devices like plates and screws inserted within the body. This method offers enhanced stability and minimizes the risk of infections, but it requires surgery and carries potential complications.
On the other hand, external fixation uses devices like rods and clamps outside the body. This approach is less invasive and can be adjusted more easily. Patients may prefer this method due to the reduced risk associated with surgery. However, external devices can be cumbersome and may lead to skin irritation or infections.
By exploring these important differences, we gain insight into the appropriate applications of each fixation method. It's essential to consider patient-specific factors, including the nature of the injury and overall health. Such knowledge empowers both doctors and patients in making informed decisions about treatment options. The nuances of fixation techniques highlight the importance of personalized care and reflect ongoing challenges in orthopedic practice.
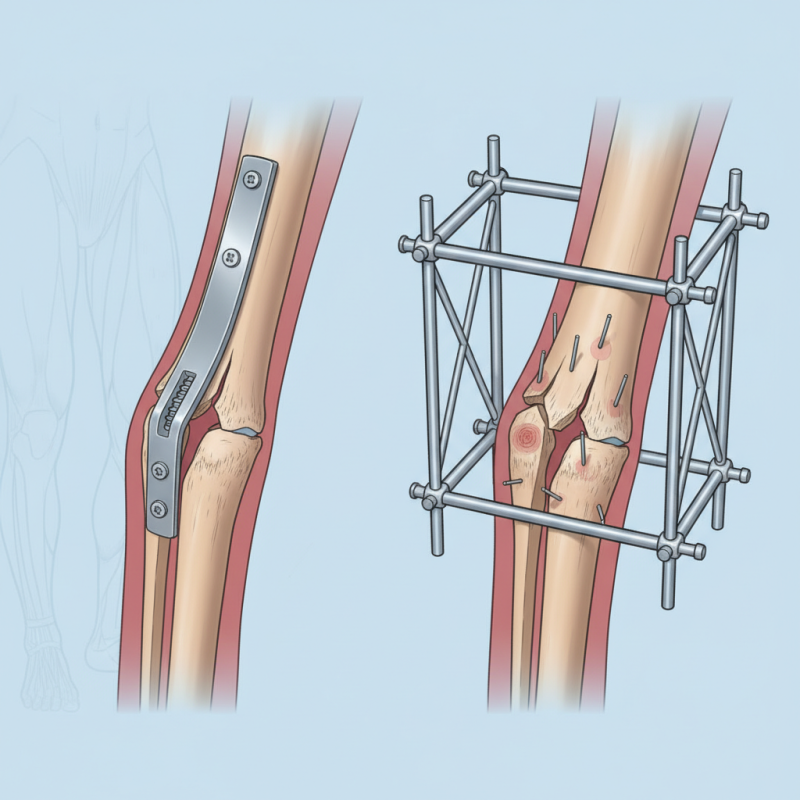
Internal and external fixation are two prominent methods for stabilizing fractures.
Internal fixation involves the surgical placement of devices inside the body to hold bones together, while external fixation uses devices outside the body. Each method has distinct advantages and drawbacks that make them suitable for different clinical scenarios.
The choice between the two often hinges on the nature of the injury. Internal fixation provides stability and allows for early mobility. A study from the Journal of Orthopaedic Trauma highlighted that patients with internal fixations had a 30% faster recovery rate compared to those using external fixation. However, surgical complications, such as infection, can occur, leading to longer recovery times in some cases. Alternatively, external fixation is less invasive and allows for easy adjustments. Yet, it can sometimes lead to improper bone alignment, requiring careful follow-up.
Each method carries risks and benefits that clinicians must weigh. While internal fixation can result in shorter healing times, external fixation's less invasive nature appeals to many surgeons. The decision also reflects individual patient circumstances, such as the type and location of fractures. Data indicates that nearly 25% of external fixation cases lead to secondary surgeries, making the choice a critical one for ongoing recovery success.
Internal fixation plays a crucial role in orthopedic surgery. This method involves the surgical placement of devices such as plates, screws, or intramedullary nails to stabilize fractured bones. Surgeons aim for precise alignment and stabilization, which can significantly enhance healing. Internal fixation is often used in complex fractures where traditional casting isn't effective.
One key principle of internal fixation is minimizing soft tissue damage.
Surgeons employ careful techniques to preserve surrounding tissues. Infection risks are also a concern. Proper sterilization and post-operative care are essential for preventing complications. Additionally, surgeons must consider factors like bone health and patient activity levels when selecting fixation methods.
Despite advancements, challenges remain. Not all fracture types suit internal fixation. Some patients may not heal as expected. Surgeons often reflect on these cases, learning to adapt techniques for better outcomes. The balance between thorough fixation and patient safety is a continuous journey in orthopedic practice.
External fixation is a unique approach to stabilizing bone fractures. This method involves devices placed outside the body, connecting to pins or screws inserted into the bones. One major benefit is the ability to keep wounds clean and accessible. The external device can also be adjusted, allowing for precise alignment during healing.
Patients often find external fixation less invasive than internal methods. There's no need for extensive surgical procedures. Recovery can be faster due to less soft tissue damage. This is particularly useful for fractures with significant soft tissue injury or infections. However, patients should be aware that wearing an external fixator can be uncomfortable and may limit mobility.
Tips: Keeping the area clean is crucial for preventing infections. Regular follow-ups with your healthcare provider help monitor healing. If pain persists, consult your doctor to reassess the treatment plan. External fixation can be effective, but each patient’s experience may vary. Therefore, it's essential to engage in open discussions with healthcare professionals to ensure the best care pathway.
Internal and external fixation techniques play crucial roles in orthopedic surgery. Each method influences the healing process differently. Internal fixation relies on surgically implanted devices, while external fixation uses appliances outside the body. This distinction leads to various outcomes in recovery times and potential complications.
Externally fixed fractures typically allow for easier monitoring and management of site infections. A 2021 study indicated that 30% of patients with external fixation experience fewer complications compared to those with internal fixation. However, external fixation may lead to longer healing times, as shown in reports indicating an average of 10-12 weeks for complete recovery.
In contrast, internal fixations generally promote a more stable environment for bones to heal. Data reveals that 75% of internal fixation patients have reduced recovery times, averaging around 6-8 weeks. They may face risks such as hardware failure or post-operative infections. Each technique requires careful consideration of individual patient circumstances, including overall health and specific fracture type. Understanding these differences is key in optimizing outcomes and addressing potential drawbacks.
When considering fixation techniques in orthopedic surgery, it is important to understand their indications and contraindications.
Internal fixation is often preferred for stable fractures where bones align well. This method provides excellent stability and allows for early mobilization.
However, it is not suitable for open fractures with significant soft tissue damage. In these cases, the risk of infection increases.
External fixation, on the other hand, is often recommended for fractures that require a more flexible approach.
It is beneficial for severe injuries where internal fixation is not feasible due to contamination or soft tissue loss.
External fixation provides easier access to the injury site. However, it can lead to complications such as pin site infections and requires diligent aftercare.
In clinical practice, the choice between these approaches is nuanced. Both methods have clear benefits but also risks that require careful consideration.
Surgeons must weigh factors like fracture type, patient health, and potential complications.
A careful evaluation ensures optimal patient outcomes while navigating the limitations inherent to each technique.
: Internal fixation involves surgically placing devices inside the body to stabilize bones.
It offers stability and allows early mobility. Patients often recover faster.
Risks include surgical complications like infections and potential hardware failure.
External fixation uses devices outside the body, making it less invasive.
It allows for easy adjustments and simpler monitoring of infections.
Yes, it can lead to improper bone alignment and longer healing times.
Recovery usually averages around 6-8 weeks for internal fixation.
External fixation may take about 10-12 weeks for complete healing.
The choice affects recovery outcomes. Misalignment or complications can arise if not chosen wisely.
Individual health, fracture type, and injury location all influence the appropriate method selection.
The article "10 Key Differences Between Internal and External Fixation" provides a comprehensive overview of the two methods commonly used in orthopedic surgery. It outlines the fundamental principles of internal fixation, which involves the use of devices implanted within the body to stabilize fractures. In contrast, external fixation utilizes devices placed outside the body, offering distinct benefits and applications based on the specific conditions of the patient.
A comparative analysis highlights the healing processes associated with both techniques, illustrating how each method has varying indications and contraindications. Ultimately, the question of what is the difference between internal and external fixation is addressed by examining their characteristics, advantages, and the specific situations where one may be preferred over the other. This detailed exploration aids medical professionals in making informed decisions tailored to individual patient needs.
