 Medisage Medical
Medisage Medical
 Medisage Medical
Medisage Medical
Fractures are common injuries that require careful treatment. The method of fixation plays a vital role in healing. Many people wonder, "why is fixation important in fracture treatment?" Fixation stabilizes the broken bones. It allows for proper alignment as they heal. Without adequate fixation, the healing process may be prolonged or complicated.
Poor fixation can lead to complications. These include malunion or nonunion of the fracture. Surgeons often use plates, screws, or rods to secure the bones. Each technique has its advantages and limitations. However, the choice depends on the fracture type and location. In some cases, patients express doubts about the fixation method. This uncertainty can stem from a lack of understanding.
Effective communication between doctors and patients is essential. Patients should feel informed and involved in their treatment decisions. Understanding the fixation process can lead to better outcomes. Many medical professionals advocate for post-treatment follow-ups. This ensures that the fixation is secure and the healing is progressing. While fixation is critical, some patients may face setbacks. Acknowledging these challenges can lead to more effective treatment strategies.
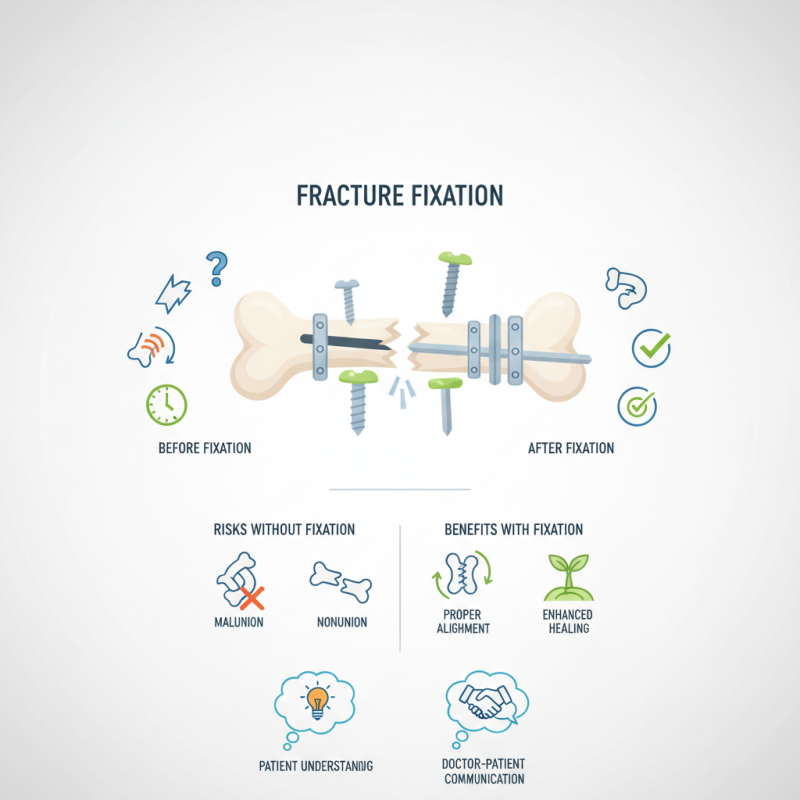
Fracture fixation plays a pivotal role in orthopedic surgery. It directly impacts patient recovery and long-term outcomes. Fixation stabilizes broken bones, allowing them to heal correctly. This is crucial because misaligned healing can lead to complications. Physicians often emphasize both surgical and non-surgical fixation methods. Each method has unique benefits depending on the fracture's type and location.
Understanding the key types of fixation helps in decision-making. Internal fixation involves implants like screws or plates. These provide solid support inside the body. On the other hand, external fixation uses devices outside the skin, offering flexibility in complex cases. The choice often depends on the fracture's severity and patient's health.
Tips: Always consult with your orthopedic surgeon on the best fixation method for your injury. Research your specific fracture type. Knowing details helps you ask informed questions. Recovery expectations vary greatly based on the fixation used. Understand that some fractures may not heal as expected; adjustments may be necessary. It’s essential to be proactive in your rehabilitation process.
Fracture fixation is essential for optimal healing. Biomechanical principles guide these techniques, ensuring that the fractured bone is stabilized. The alignment and stability of the fracture influence recovery time and outcomes. A well-fixed fracture can heal in as little as six weeks, while poorly managed cases may take months or even years.
Research shows that around 10-15% of fractures display complications. Issues arise when fixation does not provide adequate stability. Techniques like plate fixation or intramedullary nailing must consider the mechanical load and stress distribution on the bone. These choices significantly impact cellular responses and ultimately affect healing. Biomechanical analysis reveals that optimal fixation reduces the strain on healing tissues by up to 70%.
Surgeons must continuously evaluate their fixation methods. Adjustments are often needed based on patient-specific factors and fracture types. A one-size-fits-all approach rarely yields the best results. Understanding the individual biomechanics of each fracture guides effective treatment. This ongoing learning process helps improve outcomes in clinical practices, addressing the intricacies of fracture management.
Stable fixation plays a vital role in fracture healing rates. When bones break, the body initiates a healing response. However, the success of this process greatly depends on how well the broken pieces are aligned and immobilized.
Stable fixation helps maintain the correct position. This minimizes movement at the fracture site, enabling the body to mend effectively.
Research indicates that fractures treated with stable fixation heal faster than those with inadequate support. When bones are properly fixed, they can regenerate new tissue efficiently. This prevents complications such as malunion or nonunion.
Surgeons often use metal plates, screws, or rods to achieve stable fixation. Each method has its advantages and disadvantages.
For example, while plates provide broad support, they can also pose infection risks that require careful monitoring.
However, not all fractures benefit equally from surgical fixation. Some minor fractures might heal well with conservative treatment. Balancing the need for stable fixation with the risks involved is crucial. Thus, medical professionals must assess each situation individually. A nuanced understanding is necessary for optimal outcomes.
Effective fracture treatment relies heavily on the chosen fixation method. Common techniques include plates, screws, and intramedullary nails. Each has unique implications for healing and recovery. A study published in the Journal of Orthopaedic Trauma found that plate fixation resulted in a 15% lower infection rate compared to intramedullary nails in lower limb fractures. Similarly, another report indicated that adequate fixation can improve functional outcomes by 20%.
The decision on which method to use often depends on specific fracture types and patient conditions. For example, intra-articular fractures may respond better to plates due to enhanced stability. In contrast, less stable or complex fractures might be more suitable for intramedullary nailing. An assessment of 300 patients revealed that those who received targeted fixation methods reported quicker return to normal activity, emphasizing the importance of individualized treatment plans.
Tips: Always consult with a qualified orthopedic specialist to evaluate the most effective fixation method for your situation. Consider the potential complications associated with each method. Lastly, ensure proper post-operative care to promote healing and reduce the risk of re-injury. The right fixation can make all the difference in your recovery journey.
Fracture fixation technology is rapidly evolving, offering new hope to patients with bone injuries. Recent innovations focus on enhancing stability and promoting faster healing. These advancements reduce the risk of complications often seen with traditional methods. Surgeons now use bio-compatible materials that integrate well with bone. These materials help minimize inflammation and improve recovery.
In addition, minimally invasive techniques are gaining traction. These methods reduce soft tissue damage, leading to less pain and quicker rehabilitation. Surgeons can now use advanced imaging technologies for precise alignment of fractures. This approach allows for better outcomes, but it comes with a learning curve for many orthopedic professionals.
While innovations drive progress, challenges remain. Not all patients respond equally to new techniques. Factors like age and health status influence outcomes. Continuous education for healthcare providers is essential in this fast-paced field. Staying updated ensures that patients receive the best care possible, although keeping up with advancements can be daunting. The journey toward optimized fracture fixation is ongoing, filled with both promise and challenges.
: Fracture fixation stabilizes broken bones, promoting correct healing and improving recovery outcomes.
Common methods include internal fixation with implants and external fixation using devices outside the skin.
Internal fixation offers solid support inside the body, while external fixation provides flexibility for complex cases.
Knowing your specific fracture type helps you ask informed questions and enhances treatment discussions with your surgeon.
Around 10-15% of fractures may experience complications, often due to inadequate stability from the chosen fixation method.
Proper biomechanical principles reduce strain on healing tissues, leading to faster recovery times and improved patient outcomes.
The choice depends on fracture type, patient health, and potential complications linked to each fixation method.
No, a one-size-fits-all approach is rarely effective; individualized treatment based on specific biomechanics is crucial.
The fixation method used and patient-specific factors significantly impact recovery times and healing outcomes.
Be proactive in rehabilitation; some fractures may not heal as expected, so adjustments may be necessary.
Fixation is an essential aspect of fracture treatment, playing a pivotal role in ensuring optimal recovery and functional outcomes for patients. Understanding why is fixation important in fracture treatment involves recognizing its significance in stabilizing fractured bones, which directly influences the healing process. Stable fixation techniques adhere to biomechanical principles that minimize motion at the fracture site, thus promoting quicker healing rates and reducing the risk of complications.
Moreover, the comparative analysis of different fixation methods reveals varying outcomes in terms of recovery speed and long-term functionality. As advancements continue in fixation technology, orthopedic surgery is witnessing innovative approaches that enhance treatment efficacy. Ultimately, effective fracture fixation not only aids in healing but also restores mobility and quality of life for patients.
